Perilunate dislocations (see image below) and perilunate fracture dislocations are the most devastating closed injuries of the wrist.[1, 2, 3, 4, 5, 6, 7, 8] They often are missed on initial evaluation, leading to devastating complications. These injuries occur as the final stage of a spectrum of injuries progressing around the wrist in a radial-to-ulnar direction.
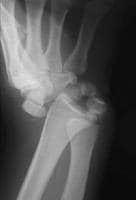 Posteroanterior plain radiograph of a dorsal perilunate dislocation. Notice the reduction of the radiolunate articulation.
Posteroanterior plain radiograph of a dorsal perilunate dislocation. Notice the reduction of the radiolunate articulation.In the setting of a high-energy wrist injury, radiographs must be scrutinized carefully for perilunate dislocation or one of its variants. Prompt open reduction with ligamentous repair or reconstruction is necessary to achieve favorable results. Posttraumatic arthrosis may result following these injuries irrespective of treatment, requiring a late salvage operation.

akibat tekanan yang hyperextension pada wrist leh la jadi cam nie....

view dari tepi plak..
Pure ligamentous perilunar injuries of the wrist are classified as lesser arc injuries, while the transosseous variants are regarded as greater arc injuries. The mechanism of perilunate dislocations has been described as a 4-stage process, as follows:
- First stage - The RSC ligament and the scapholunate interosseous ligament rupture.
- Second stage - Dislocation of the capitolunate joint occurs as the injury progresses through the space of Poirier.
- Third stage - The lunotriquetral interosseous ligament ruptures.
- Fourth stage - The lunate becomes dislocated.
This mechanism has been reproduced in a cadaver model by applying pronation and ulnar deviation on a hyperextended cadaver wrist.

haa tgk cmne tgn dia..
SURGICAL THERAPHY
Surgical options include the following:
- Closed reduction and casting
- Closed reduction and percutaneous pin fixation
- Open reduction and open ligamentous repair with internal fixation or with percutaneous pin fixation
The surgical treatment of choice is open reduction and ligamentous repair with percutaneous pin fixation.
Once informed consent has been obtained and the surgeon has again identified the affected extremity, the patient is taken to the operating room. The patient is positioned supine on the operating room table, and the affected extremity is placed on a radiopaque hand table. Because the duration of the procedure may be long, padding should be placed beneath the knees and heels, and the use of a Foley catheter should be considered. An upper arm tourniquet is applied, being well padded, and the tourniquet is inflated after the arm is prepared and draped.
Attention is turned first to the dorsum of the wrist, where a midline longitudinal incision is made and the extensor retinaculum is exposed.
See image below.
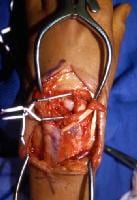 Dorsal approach to the wrist demonstrating disruption of the scapholunate interosseous ligament.
Dorsal approach to the wrist demonstrating disruption of the scapholunate interosseous ligament.The extensor retinaculum is divided between the third and fourth dorsal compartments, and the dorsal wrist capsule is exposed. The dorsal radiotriquetral and dorsal intercarpal ligaments are identified. A radially based, dorsal V capsulotomy is performed, with the base of the V at the intersection of the dorsal intercarpal and radiotriquetral ligaments. This capsulotomy preserves these dorsal ligamentous structures, which are known to play a role in the stability of the wrist, as seen in the images below.
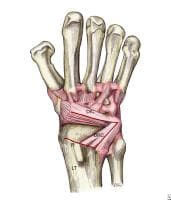 Capsulotomy approach to the scapholunate interosseous interval, with preservation of the dorsal intercarpal and dorsal radiocarpal ligaments. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).
Capsulotomy approach to the scapholunate interosseous interval, with preservation of the dorsal intercarpal and dorsal radiocarpal ligaments. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).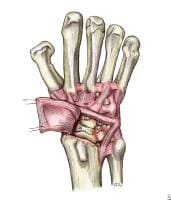 Reflected dorsal wrist capsulotomy preserving the dorsal intercarpal and dorsal radiocarpal ligaments. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).
Reflected dorsal wrist capsulotomy preserving the dorsal intercarpal and dorsal radiocarpal ligaments. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).Through this capsulotomy, accurate reduction of the radiocarpal and midcarpal joints is accomplished. It is imperative that the scaphoid be contained securely in the scaphoid fossa and that the lunocapitate articulation be reduced completely. The lunate is derotated from its dorsal position and is stabilized with a 0.062 Kirschner wire (K-wire), which is directed from the radial styloid into the body of the lunate.[20] The lunate reduction is extremely important, because after the lunate is reduced, the remainder of the carpus can be reconstructed. See image below.
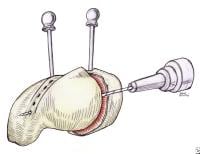 Drawing showing the reduction of the scapholunate interval using Kirschner wire (K-wire) joysticks. Drill holes are made using straight needles for subsequent passage of suture. This scapholunate repair technique was originally described by Taleisnik.
Drawing showing the reduction of the scapholunate interval using Kirschner wire (K-wire) joysticks. Drill holes are made using straight needles for subsequent passage of suture. This scapholunate repair technique was originally described by Taleisnik.The scapholunate ligament is identified, and 1 of 2 methods is chosen for ligamentous repair. One option is the placement of 2 small suture anchors into the defect of the scaphoid proximal pole. This defect typically is created following avulsion of the scapholunate interosseous ligament. The accompanying suture attached to the suture anchors can then be placed through the scapholunate ligament, with the ligament secured once the scapholunate interval is reduced. See image below.
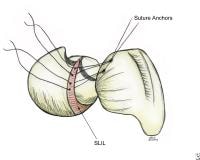 Drawing demonstrating suture anchor placement for the repair of the scapholunate interosseous ligament. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).
Drawing demonstrating suture anchor placement for the repair of the scapholunate interosseous ligament. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).Alternatively, 2 small drill holes are created from the defect in the proximal pole, exiting at the waist of the scaphoid along its radial ridge. These drill holes are created with a 2-mm drill, and a 2-0 nonabsorbable suture is placed through the scapholunate interosseous ligament. Once reduction of the scapholunate interval is ensured, a pair of 0.045 K-wires is advanced from the scaphoid into the lunate. A third wire is passed from the midwaist region of the scaphoid into the waist region of the capitate. Once the reduced scapholunate interval is secured, the sutures may be tied. See images below.
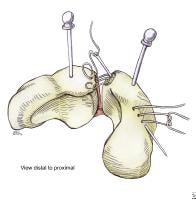 Drawing showing repair of the scapholunate interosseous ligament using drill holes and suture passed with straight needles, as described by Taleisnik. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).
Drawing showing repair of the scapholunate interosseous ligament using drill holes and suture passed with straight needles, as described by Taleisnik. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).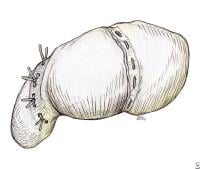 Drawing showing the final repair of the scapholunate interosseous ligament using drill holes, as described by Taleisnik. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).
Drawing showing the final repair of the scapholunate interosseous ligament using drill holes, as described by Taleisnik. Image adapted from The Wrist: Diagnosis and Operative Treatment (Mosby, 1998).Similarly, an attempt may be made to repair the lunotriquetral interosseous ligament, although generally this is technically difficult. The surgeon often resorts simply to pinning the lunotriquetral interval percutaneously. The midcarpal articulation is stabilized with the pinning of the scaphoid to the capitate.
In the transosseous variants of the perilunate dislocation, providing internal fixation of the fractures is preferable. Scaphoid fractures, for example, should be reduced and stabilized with a cannulated compression screw, as should capitate fractures. Radial styloid fractures, triquetral fractures, and smaller varieties of capitate or scaphoid fractures may be better suited for reduction and stabilization with percutaneous K-wire fixation. The placement of percutaneous K-wires, as well as the assessment of the midcarpal joint reduction or of the scapholunate interval reduction, is carried out with intraoperative fluoroscopy.
Once the perilunate dislocation or the perilunate fracture dislocation has been reduced and stabilized successfully, attention is turned to the volar aspect of the wrist. An extensile carpal tunnel approach is used to expose the volar wrist capsule, and the carpal tunnel is released. A transverse rent in the volar wrist capsule is routinely found and should be repaired with 2-0 nonabsorbable suture. See image below.
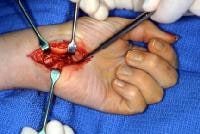 Volar wrist approach for the repair of the transverse capsular rupture, an injury that is typically seen in perilunate dislocations.
Volar wrist approach for the repair of the transverse capsular rupture, an injury that is typically seen in perilunate dislocations.The tourniquet is released prior to closure, and the wounds are closed once hemostasis is obtained. A sterile dressing is applied, followed by a well-padded volar plaster splint. External fixation should be considered in the setting of marked swelling or open wounds. It should also be considered when patient compliance is a concern or fixation stability is in question.
Following surgery, the hand should be elevated for 48 hours and the neurologic and vascular status should be monitored. Overnight admission to the hospital is recommended. A small pullout drain generally is recommended for both wounds. Sometime between postoperative days 3 and 5, the dressing and splint should be removed so that the wounds can be examined. At 10-14 days, the sutures are removed, and a short arm cast is applied. See radiograph below.
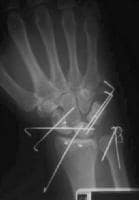 Postoperative posteroanterior radiograph following open reduction and percutaneous pinning of a dorsal perilunate dislocation. Note that suture anchors have been placed in the scaphoid to directly repair the scapholunate interosseous ligament. Suture anchors have also been used in the distal radius to perform a capsulodesis using the dorsal intercarpal ligament.
Postoperative posteroanterior radiograph following open reduction and percutaneous pinning of a dorsal perilunate dislocation. Note that suture anchors have been placed in the scaphoid to directly repair the scapholunate interosseous ligament. Suture anchors have also been used in the distal radius to perform a capsulodesis using the dorsal intercarpal ligament.Following open reduction and ligamentous repair of the perilunate dislocation, the cast is maintained for 3 months. Radiographs are obtained periodically to ensure maintenance of midcarpal and radiocarpal reduction. Upon cast removal, the patient is placed in a removable splint, and gentle range-of-motion exercises are begun. Splinting is continued until 6 months postsurgery. Full activity is not renewed until 8 months postsurgery.
ok thats all...article nie diambil dari...rujukan yang lebih lanjut leh search sendiri yer!!
http://emedicine.medscape.com/article/1240108-workup#a0721
p/s : kepada yang berkenaan : semoga cepat cihat.. :)
































0 comments:
Post a Comment